Karla Salp
Communications
 |
| Pigs with their curly tails in a pasture |
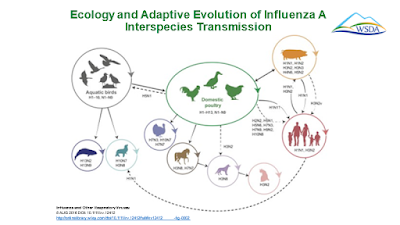
Influenza viruses can be passed between humans, birds, and pigs.
Because of this, it is important to practice good biosecurity whenever
interacting with either birds or pigs on your farm and when attending fairs and
livestock shows.
Swine flu viruses are different from seasonal flu viruses that infect people. Flu vaccines don’t generally protect against swine flu; they protect people against seasonal flu, which can also spread to pigs.
No swine flu vaccine is available for animals yet in the United States, but
work is being done to get an approved vaccine to use for control in the face of
an outbreak, with promising vaccines demonstrating 100% efficacy in swine.
Swine flu can spread among pigs throughout the year, though
rates increase significantly when infected pigs spend more than three days at a
fair or livestock show. Reducing the time pigs spend at fairs to three days or
less is one way to reduce the risk of spreading swine flu. The Swine Exhibitions
Zoonotic Working Group has also produced a checklist for exhibition organizers
and youth organization leaders to minimize
the spread of influenza, which includes recommended actions to take before,
during, and after exhibitions.
 |
| Pig in a pen at a fair |
- Avoid close contact with pigs that look or act
ill. For exhibition organizers, pigs should be observed daily for flu-like
symptoms.
- Wash your hands with soap and running water before and after contact with pigs or visiting a swine barn or exhibit. Use an alcohol-based hand rub if soap and water are not available.
- People that are 65 or older, children under the age of 5, people who are pregnant, and people with certain long-term health conditions have higher risk of serious flu complications and should consider avoiding pigs and swine barns.
- Keep food, drinks, and baby items, such as toys, pacifiers, bottles, and strollers, out of areas where there are pigs.
“After the fair, don’t bring home more than that blue
ribbon,” Dr. Amber Itle, Washington State Veterinarian, said. “When showing
animals – especially pigs and birds – take extra precautions to
prevent the spread of swine flu and other diseases.”
But don’t think it is just the pigs that can infect humans.
Humans can also infect pigs, so if you are not feeling well, take precautions
to prevent spreading disease to your animals or have someone else care for your
animals until you feel better.
If you own both birds and pigs, they should always be kept separate to reduce the risk of infection and mutating viruses. Prior to COVID-19, the last global pandemic was swine flu in 2009 – infecting an estimated 60 million people and resulting in over 12,000 deaths in the United States alone. That strain had signs of combined human, bird, and swine origins.
Given the high numbers of detection of bird flu throughout
the country this year, adding swine flu to the mix is an unwelcome prospect –
increasing the risk of another infectious and potentially deadly influenza
strain. Keeping pigs and birds separated and practicing good biosecurity could
prevent the next pandemic.
Additional resources
Take
Action to Prevent the Spread of Flu Between Pigs and People | CDC
Key Facts about
Human Infections with Variant Viruses | CDC
What
People Who Raise Pigs Need To Know About Influenza (Flu)